Diabetic Neuropathy is one of the most prevalent complications of diabetes, impacting nearly half of all individuals with the condition at some stage of their lives. This progressive nerve disorder results from sustained high blood sugar levels, which gradually damage nerves throughout the body. Prompt detection and proactive management are essential to reduce the risk of serious complications, including foot ulcers, infections, and impaired mobility. At Cherry Medical, we offer expert guidance and personalized treatment plans to help patients effectively manage diabetic neuropathy and maintain a healthier, more active life.
Call Cherry Medical today at (714) 819-0000 for fast and effective Diabetic Neuropathy Treatment.
What is Diabetic Neuropathy?
Diabetic neuropathy is a type of nerve damage that occurs as a complication of diabetes. It develops when high blood sugar levels persist over time, causing injury to the nerves throughout the body. The condition most commonly affects the feet, legs, hands, and arms, but it can also impact internal organs.
There are several types of diabetic neuropathy, each with unique symptoms and effects:
- Peripheral Neuropathy: Affects the extremities, leading to pain, tingling, or numbness.
- Autonomic Neuropathy: Impacts organs such as the heart, bladder, and digestive system.
- Proximal Neuropathy (Diabetic Amyotrophy): Causes sudden pain and muscle weakness in the thighs, hips, or buttocks.
- Focal Neuropathy (Mononeuropathy): Involves sudden nerve damage in a specific area, such as the face, torso, or eyes.
If left untreated, diabetic neuropathy can lead to serious complications, including foot ulcers, infections, balance problems, and reduced quality of life. Early diagnosis and proper management are key to slowing progression and preventing long-term damage.
Diabetic Neuropathy Causes, Symptoms and Diagnosis
Diabetic neuropathy is a progressive nerve disorder primarily caused by prolonged high blood sugar levels. Understanding its causes, common symptoms, and diagnostic methods is essential for early detection and effective management. At Cherry Medical, we provide comprehensive guidance and scientifically accurate information to help patients better understand diabetic neuropathy and receive timely medical care.
The table below offers a clear overview of the main causes, typical symptoms, and recommended diagnostic approaches for diabetic neuropathy:
| Causes of Diabetic Neuropathy | Symptoms of Diabetic Neuropathy | Diagnosis of Diabetic Neuropathy |
|---|---|---|
| Chronic high blood sugar (Hyperglycemia) | Peripheral Neuropathy: Tingling, burning, or sharp pain in hands or feet; numbness; sensitivity to touch; muscle weakness; slow-healing foot wounds | Blood sugar tests, HbA1c levels |
| Long duration of diabetes | Peripheral & Proximal Neuropathy: Numbness, weakness in extremities; difficulty standing or walking; sudden pain in thighs, hips, or buttocks | Neurological examination, detailed patient history |
| Obesity & sedentary lifestyle | Muscle weakness, poor coordination, balance issues | Physical examination, reflex tests |
| High blood pressure & high cholesterol | Sensitivity to touch, numbness, slow healing | Cardiovascular assessment, blood pressure & lipid panel |
| Smoking & excessive alcohol consumption | Slow-healing foot wounds, infections | Foot inspection, skin evaluation |
| Kidney disease | Autonomic Neuropathy: Digestive issues (nausea, diarrhea, constipation) | Kidney function tests, urinalysis |
| Nerve compression or injury | Autonomic & Focal Neuropathy: Urinary problems (incontinence, retention); facial or eye-related nerve issues | Nerve conduction studies, EMG |
| Age & genetic predisposition | Autonomic Neuropathy: Sexual dysfunction; irregular heart rate or blood pressure | ECG, autonomic function tests |
Learn the Early Signs of Neuropathy and Find Out When to Visit a Neurologist in Orange County!
Diabetic Neuropathy Treatment
Treating diabetic neuropathy focuses on managing symptoms, slowing disease progression, and preventing complications. Early intervention is crucial to improve quality of life and reduce the risk of serious outcomes such as foot ulcers, infections, or mobility issues.
- Blood Sugar Control
Maintaining optimal blood glucose levels is the most effective way to prevent further nerve damage in diabetic neuropathy. Patients can achieve this through a combination of lifestyle measures, including a healthy, balanced diet, regular physical activity, and proper weight management. In addition, medications such as insulin or prescribed oral antidiabetic drugs play a crucial role in keeping blood sugar within target ranges. By controlling glucose levels consistently, patients can slow the progression of neuropathy, reduce symptoms, and lower the risk of serious complications such as foot ulcers and infections.
- Medications for Symptom Relief
Medications play a key role in managing the pain associated with diabetic neuropathy. Antidepressants such as Duloxetine and Amitriptyline can help reduce nerve pain by affecting pain-signaling pathways. Anticonvulsants, including Gabapentin and Pregabalin, are also effective in controlling neuropathic pain and improving quality of life. For mild discomfort, pain relievers like Acetaminophen or NSAIDs may be recommended. Combining these medications with proper blood sugar management and lifestyle measures can provide comprehensive relief and slow the progression of nerve damage.
- Topical Treatments
Topical treatments can provide targeted relief for patients with diabetic neuropathy. Capsaicin cream is often used to reduce localized burning or tingling sensations by desensitizing nerve endings, while lidocaine patches offer precise pain management for specific affected areas. These topical options, when combined with proper blood sugar control and other therapies, can significantly improve comfort and daily functioning for patients suffering from neuropathic pain.
- Physical Therapy & Exercise
Physical therapy and regular exercise play a vital role in managing diabetic neuropathy. They help improve muscle strength, coordination, and balance, which reduces the risk of falls and mobility issues. Additionally, consistent physical activity has been shown to reduce neuropathic pain and enhance overall functional independence, making daily activities easier and more comfortable for patients. Incorporating exercise into a comprehensive treatment plan can significantly improve quality of life.
- Lifestyle Modifications
Lifestyle modifications are essential for managing diabetic neuropathy and preventing complications. Daily foot care and wearing proper footwear help protect against injuries, infections, and slow-healing ulcers. Avoiding smoking and limiting alcohol consumption can improve blood flow and nerve health, while a balanced diet rich in fiber and low in refined sugars supports overall glucose control and reduces the risk of further nerve damage. Combined with medical treatments and regular monitoring, these lifestyle measures play a crucial role in maintaining long-term health and quality of life.
- Advanced Treatments
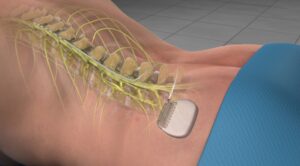
In severe cases of diabetic neuropathy, there are a few options to decrease the discomfort. Low-dose naltrexone has shown promising results in some of these patients. We may also use ketamine infusion to reduce the pain associated with this pain. A spinal cord stimulator is another super-effective treatment to control the pain. Programs combining advanced medications, physical therapy, and targeted interventions provide comprehensive relief, improve mobility, and enhance quality of life for individuals with challenging neuropathy symptoms.

Diabetic Neuropathy Treatment at Home
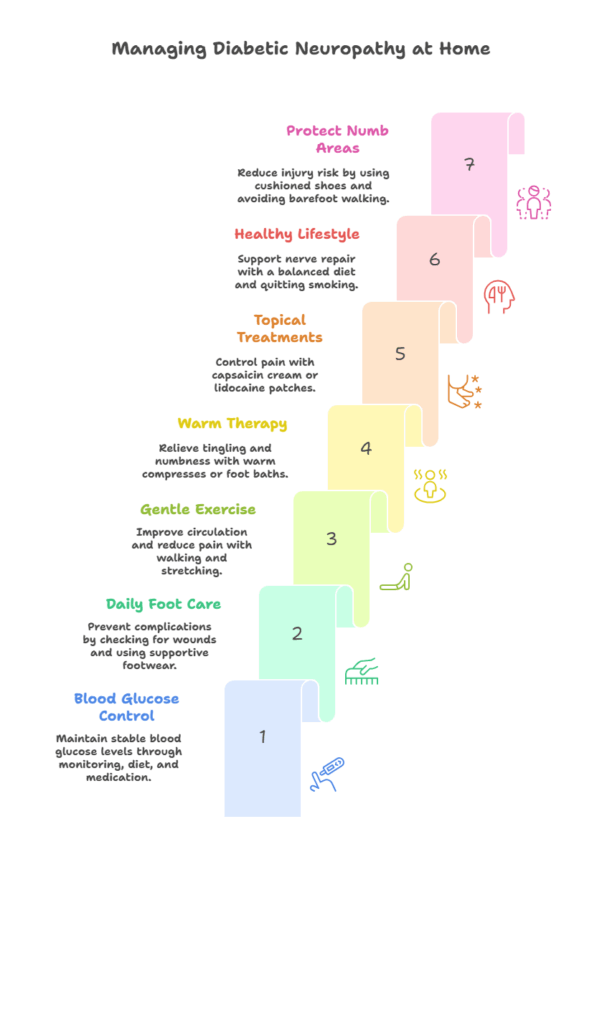
At Cherry Medical, we provide a range of effective at-home strategies to help patients manage diabetic neuropathy, protect nerve health, and reduce daily discomfort. Maintaining stable blood glucose levels through regular monitoring, a balanced diet, and proper medication use is the most essential step in slowing nerve damage. Daily foot care (including checking for wounds, washing and drying carefully, and using supportive footwear) helps prevent serious complications. Gentle exercises such as walking and stretching improve circulation, strengthen muscles, enhance balance, and reduce neuropathic pain.
Warm compresses or warm (not hot) foot baths can offer temporary relief from tingling and numbness. For targeted pain control, topical treatments like capsaicin cream or lidocaine patches are often helpful. Adopting healthy lifestyle habits, including quitting smoking, limiting alcohol, and following a fiber-rich, low-sugar diet, supports nerve repair and better blood flow. Protecting numb areas with cushioned shoes and avoiding walking barefoot further reduces the risk of injury. By combining these home-based methods with regular follow-ups at Cherry Medical, patients can significantly improve their comfort, mobility, and overall quality of life while living with diabetic neuropathy.
FAQs about
At Cherry Medical, we understand that living with diabetic neuropathy can bring many questions about symptoms, treatment options, and prevention strategies. To help you manage this condition effectively, we have compiled clear and concise answers to the most frequently asked questions by our patients. This FAQ section covers essential topics such as foot care, medications, lifestyle adjustments, and expert recommendations, providing reliable guidance to support nerve health and improve your overall quality of life. For further guidance or personalized medical advice, Contact Us at Cherry Medical.
Are there natural or lifestyle remedies that help with diabetic neuropathy?
Yes. exercise, a healthy diet, quitting smoking, limiting alcohol, controlling blood pressure and cholesterol, and foot care are very effective.
How important is blood sugar control in preventing or slowing down neuropathy?
It’s the most important factor. tight glucose control is key to slowing nerve damage and reducing symptoms.
Can exercise help with diabetic neuropathy?
Yes. regular, moderate-intensity exercise improves circulation, lowers blood sugar, strengthens muscles, and can reduce neuropathic pain.
What is the best treatment for diabetic neuropathy in feet?
A combination of blood sugar control, pain medications (gabapentin, pregabalin, duloxetine), topical creams (lidocaine, capsaicin), and proper foot care is most effective.
Can diabetic neuropathy be reversed?
Complete reversal is rare, but early blood sugar control and lifestyle changes can improve symptoms and slow progression. Some patients report symptom improvement with tight glucose control, healthy habits, and treatment, though full nerve regeneration is unlikely.
How can I prevent diabetic neuropathy?
Maintain stable blood sugar, follow a balanced diet, exercise regularly, avoid smoking, limit alcohol, and practice daily foot care to reduce risk.
How often should diabetics check their feet for prevention?
Daily self-inspection for cuts, blisters, or redness, plus annual professional foot exams, helps detect problems early and prevent complications.
Does neuropathy affect all diabetics or only those with poor glucose control?
While poor glucose control heightens the risk, not everyone with diabetes develops neuropathy. Other factors, like kidney disease or vascular issues, can also contribute.
Are there surgical options for severe diabetic neuropathy?
While there’s no cure, some cases may benefit from specialized interventions; for example, to relieve pressure on nerves or manage severe complications.
Can diabetic neuropathy affect other organs besides the feet, like the digestive system or heart?
Yes. the autonomic type of neuropathy can impact digestion (gastroparesis), bladder function, blood pressure regulation, and even sexual function.
What are the side effects of neuropathy medications like Gabapentin or Duloxetine?
Common side effects of Gabapentin or Pregabalin include dizziness, drowsiness, and swelling. Antidepressants like Duloxetine may cause nausea, fatigue, or drops in blood pressure.
What medications are commonly used for diabetic neuropathy pain relief?
Common medications include anticonvulsants (like Gabapentin, Pregabalin) and antidepressants (like Duloxetine, Amitriptyline). For topical pain, lidocaine patches or capsaicin cream can also be used.
Can exercise help with diabetic neuropathy?
Yes. regular, moderate-intensity exercise improves circulation, lowers blood sugar, strengthens muscles, and can reduce neuropathic pain.
When should someone see a specialist for diabetic neuropathy?
You should consult a specialist if you have painful symptoms, foot sores that won’t heal, digestive or bladder issues, or if neuropathy significantly affects your quality of life.
What type of doctor should I see for diabetic neuropathy?
For diabetic neuropathy, visit an endocrinologist (diabetes specialist) for blood sugar management and a neurologist for nerve assessment and pain management. A podiatrist is also recommended for foot care and prevention of complications.
Dr. Alireza Bozorgi is a board-certified neurologist and pain management specialist with over 20 years of clinical and research experience. He has completed multiple fellowships and residencies in neurology and pain management, holds active medical licensure in California, and has published numerous peer-reviewed research papers.
For full details on Dr. Bozorgi’s education, certifications, work experience, and publications, view his complete CV here.
How can I book an appointment at Cherry Medical?
You can easily book an appointment with Dr. Alireza Bozorgi at Cherry Medical by:
- Calling us: (714) 819-0000
- Online booking:
- visit our website, “www.cherrymedical.org“ and fill out the appointment request form
- book online in the scheduling website at “http://www.patientfusion.com/doctor/alireza-bozorgi-30060“
- send us an email at “ask@cherrymedical.org“